2. The Science of Addiction
Contents
HOW SUBSTANCES AFFECT THE BRAIN – THE SCIENCE BEHIND IT
All humans (and other animals) possess survival related drives, such as eating, sleeping, socializing and procreating. Because these behaviours are essential to our survival, a system exists within the brain that marks them as rewarding, which reinforces these behaviours and makes us more likely to repeat them. This is known as the reward pathway. Dopamine, a chemical signal in the brain (a neurotransmitter), is the key ingredient in the reward system.
Insights from animal and human research studies suggest that psychoactive substances alter this reward system. Stimulants and empathogens directly increase dopamine levels, while depressants and opioids indirectly increase dopamine levels. These substances cause dopamine to be released in the reward pathway, which reinforces the behaviour of taking the substance.[5]
To learn more about the effects of opioids on your brain, watch this video:
When substances are taken frequently and regularly, brain circuits, including the reward system, adapt over time. Because of their effect on the reward system, the brain comes to think that the substances are essential for our survival and become necessary to feel normal. Other pathways also adapt to drive negative mood states and cravings when the substance is not taken. These pathways can lead to excessive ‘wanting’ even if the individual no longer experiences pleasure from using the substance.[6]
TYPES OF SUBSTANCES AND THEIR EFFECTS






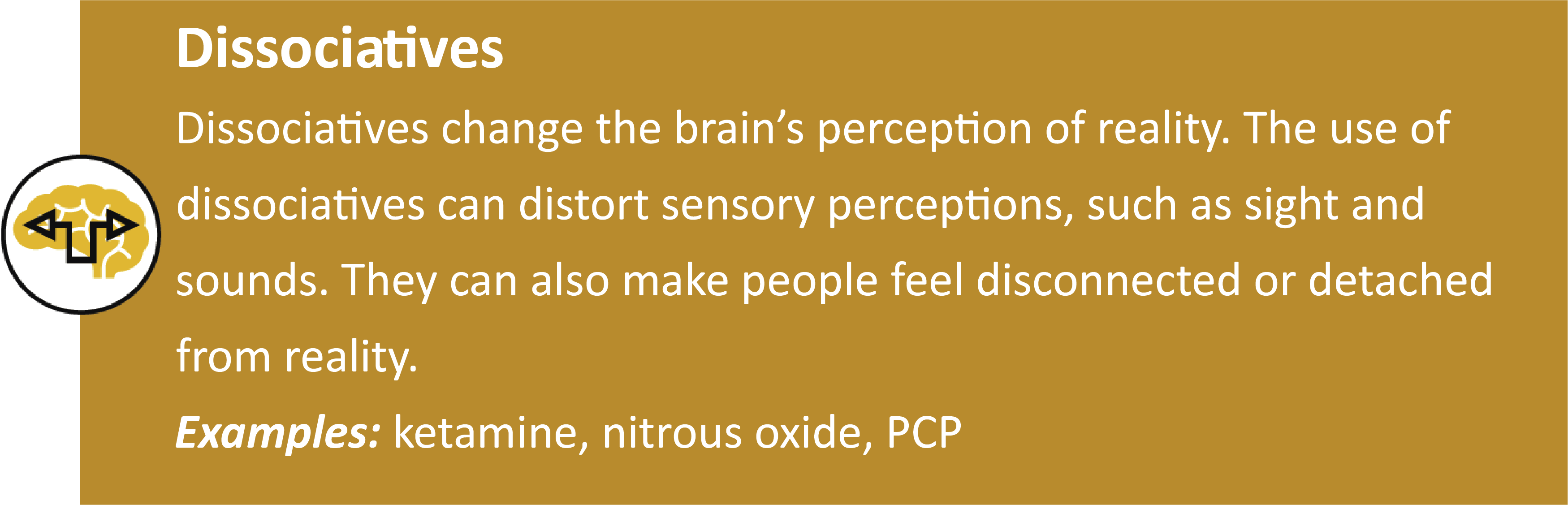
For more information about the effects of different substances see the Alcohol and Drug Foundation’s Interactive Drug List and Wheel.[7]
THE DEVELOPING BRAIN
Young people are particularly vulnerable to the effects of substances because their brains are still developing. The prefrontal cortex, which plays a role in decision-making, emotional regulation and impulse control, is not fully developed until their mid-20s, so they are naturally more prone to risktaking behaviour.
There may be a lack of impulse control tied to the substance use and addiction among young people. Young people are granted independence and freedom but there is still a judgment gap. To learn more about the developing brain in young people and how it relates to substance use, check out the video from the National Institute on Drug Abuse, about Teen Brain Development.[8]
SUBSTANCE USE CONTINUUM
Substance use disorder is a chronic relapsing health condition that can impact anyone, regardless of socioeconomic status. The reasons people develop substance use disorders are complex. Often, there is a combination of biological, psychological and social factors that can contribute to your young person’s substance use. Risk factors include genetic predispositions, adverse childhood experiences (ACEs), negative social influences, and mental health disorders.[9]
It can take a long time for your young person to get better. Recovery is not a linear process and relapses are often a part of it, just like many other chronic health conditions. This can feel discouraging to hear, however it’s important to remember that recovery is a lifelong journey. Your young person will need to develop coping skills to deal with stressors, thoughts, and cravings. This will become easier with time and practice.
RECOVERY CAPITAL
The more resources your young person has to support their recovery, the easier it will be to maintain. We call this recovery capital. It can include things like supportive relationships, nutrition, sleep, school, work, selfesteem, and life meaning. If a young person has high recovery capital, they may require fewer resources to prevent relapses, while those who have low recovery capital may require more treatment services and supports.[10]
Take a deeper dive into these concepts by exploring the following resources:
Canadian Centre on Substance Use and Addiction: Presents five concepts critical to understanding adverse childhood experiences and their impact on brain development and health.
Alberta Family Wellness Initiative: The AFWI has a library of free resources for anyone to use and share.

Footnotes
[5] Nestler, E.J. (2005). Is there a common molecular pathway for addiction? Nature Neuroscience, 8: 1445-49.
[6] Koob, G.F. & Volkow, N.D. (2016). Neurobiology of addiction: a neurocircuitry analysis. Lancet Psychiatry, 3:760-73.
[7] Alcohol and Drug Foundation. (April 23, 2021). Drug Wheel. Available at: https://adf.org.au/drug-facts/#wheel
[8] Available at: www.youtube.com/watch?v=EpfnDijz2d8&feature=emb_logo
[9] Whitesell, M., Bachand, A., Peel, J., & Brown, M. (2013). Familial, social and individual factors contributing to risk for adolescent substance use. Journal of Addiction Medicine, 2013:578310.
[10] White, W.L. & Cloud, W. (2008). Recovery capital: A primer for addictions professionals. Counselor, 9(5):22-7.
